
We can envision a future in which everyone has the same prospects for living a long and healthy life, no matter who they are or where they call home. All people live in safe and healthy environments. We all enjoy reliable access to health care, nutritious food, and stable housing. We have the knowledge and opportunity to make healthy choices about diet and exercise. And no one has to contend with the harms of persistent racial discrimination, violence, trauma, despair, and injustice.
Realizing this vision of equity in healthy life expectancy requires bold actions by the health care sector, government, business, and philanthropy. The health care sector plays a central role, starting with developing federal and state policies that make health care available, accessible, and affordable for everyone. And routine screening, diagnosis, and treatment for mental, behavioral, and physical health problems are essential. But institutions that deliver and pay for health care also play a part in helping patients address the social needs that so profoundly influence health and well-being.
The challenge is urgent. Health inequities by race, ethnicity, and socioeconomic status exist at every stage of life, accumulate over time, and affect both the length and quality of people’s lives. As of 2017, for example, non-Hispanic black men’s life expectancy was 4.5 years shorter than that of non-Hispanic white men. Among women, the gap was 2.7 years. And since about 1980, the US has seen a widening gap in life expectancies between rich and poor people.
Looking ahead, stagnating wages and hardship among those at the bottom of the economic ladder threaten to worsen the mortality rate and prevalence of chronic diseases. This could be further exacerbated by an aging population, which is likely to raise the rates of chronic disease in the population as a whole and escalate competing demands on government income support and health programs. And if disparities in health and longevity between racial and ethnic groups persist as our nation becomes more diverse, growing burdens of chronic disease and premature death could further increase government spending on health care in the decades ahead.
Health-Related Social Needs: Promising Solutions
Across the country, health care providers and public, private, and nonprofit payers are exploring solutions to help people meet their health-related social needs, particularly among Medicaid enrollees. Along the way, they are generating new insights and raising critical questions about what works. Below, we highlight five bold approaches that could narrow inequities in health outcomes and healthy life expectancy.

Photo by Katherine Frey/The Washington Post via Getty Images.
“Social barriers, such as housing instability and quality, food insecurity, personal safety, and lack of transportation and affordable utilities, affect people’s ability to maintain their health and well-being. This [Accountable Health Communities] award will enable UnitedHealthcare and our clinical partners to identify the needs of some of our most vulnerable residents and connect them to community-based organizations that can help them live healthier lives.”
— Katherine Keir, UnitedHealthcare Hawaii State Director
Assess health-related social needs
Some major health care providers and payers have started to routinely ask clients about their social needs along with their health needs. The move can reveal key drivers of health inequities and marks a critical first step for targeted referrals for and investments in nonmedical services that can improve health and life expectancy.
- The federal Accountable Health Communities demonstration requires health care providers to identify health-related social needs using a standardized screening tool that is being implemented in hundreds of communities.
- Community health centers around the country use the Protocol for Responding to and Assessing Patient Assets, Risk, and Experiences (PRAPARE) to ask their patients about their housing worries and whether they can pay for food, utilities, clothing, child care, and transportation.
Build community resource networks
Efforts to implement and standardize screening for social needs in health care settings need to go hand in hand with referral systems that connect patients to services and track what happens to them. Several promising efforts are under way to develop, finance, and maintain community resource networks and platforms.
- North Carolina’s statewide electronic care coordination network called NCCARE360 combines health care and social service organizations (including a dedicated call center and data team to verify the information) with a referral platform that enables health care and social service providers to securely exchange data and monitor outcomes.
- The nonprofit 2-1-1 San Diego provides phone- and web-based care coordination through a team of health navigators. It also includes a cloud-based interactive database that allows participating health care and social service providers and government agencies to securely exchange information.
- Kaiser Permanente launched its Thrive Local initiative to link its members to services and supports in their communities. The “social care network” will be integrated into Kaiser Permanente’s electronic health records and will track referrals and outcomes to assess how well people’s needs are being met.
Although online resource network platforms are spreading, not every community has the infrastructure for electronic data exchange and coordination, so some are implementing alternative solutions.
- Colorado’s Regional Health Connectors program employs community members to link primary care providers with community-based behavioral health and social service organizations.

Photo by Stephen Voss.
“We know that behaviors and other determinants of health—like where we work, live, learn, and grow—are all factors in our overall health and well-being…. North Carolina will implement a groundbreaking program in select regions to pilot evidence-based interventions addressing issues like housing instability, transportation insecurity, food security, and interpersonal violence and toxic stress.”
— Seema Verma, Administrator of the Centers for Medicare & Medicaid Services, “CMS Approves North Carolina’s Innovative Medicaid Demonstration to Help Improve Health Outcomes,” HealthAffairs
Incentivize investments in nonmedical services with health payoffs
Health care providers and plans need appropriate financing mechanisms to play a sustained role in addressing health-related social needs. Federal and state governments are testing ways to require or reward nonmedical investments that improve people’s health or reduce medical costs.
Some state Medicaid programs require managed care organizations they contract with to address clients’ social needs or to support community-based organizations that do.
- Arizona requires managed care organizations to reinvest 6 percent of any profit or surplus in the community. Similarly, in 2020, Oregon will require its coordinated care organizations to spend a portion of any year-end surplus or excess reserves on addressing health disparities and people’s social needs.
- Also in 2020, Massachusetts will require its accountable care organizations to offer members “flexible services” that address social needs, such as having a safe and healthy living environment.
Some states are using new payment models and incentives to provide nonmedical services.
- Medicaid health plans in Minnesota and Louisiana must select and report their performance on at least one incentive-based quality measure related to improving health equity and population health, including using data on social needs.
Provide sustainable financing
Health care providers and payers can play an important role in addressing their clients’ health-related social needs, but they might not financially benefit from doing so. In fact, returns on investment may accrue to other public- and private-sector entities. So, in addition to realigning incentives within the health sector, policymakers are considering cross-sector approaches and ways to sustain them.
One promising solution is to pool or coordinate funding from multiple government programs that serve the same people.
- Virginia’s Children’s Services Act, passed in 1993, combines state funds across education, juvenile justice, and other social service agencies and allocates them to communities where they are managed by a locally appointed team to fund services for at-risk children and youth.
- Many other states have established “children’s cabinets,” collaborative coordinating bodies that bring together agencies with overlapping goals but separate funding streams.
Several philanthropic and venture capital initiatives support cross-sector and public-private collaborations to improve health and health equity in targeted communities.
- The Magnolia Place Community Initiative brings together residents and community-based service providers in four neighborhoods of South Central Los Angeles to improve child and family well-being. As part of this initiative, multiple service agencies are housed in the same community center, allowing them to collaborate in real time and improving the chances they can address residents’ diverse social needs in a timely manner.
- The Build Healthy Places Network supports communities in developing sustainable collaboration between public and private finance, community development, and health organizations to promote health equity.
- Other partnerships—including pay for success approaches and community-based models, such as the newly developed Collaborative Approach to Public Good Investments—also aim to foster cross-sector collaborations and increase investments in areas where benefits are shared.
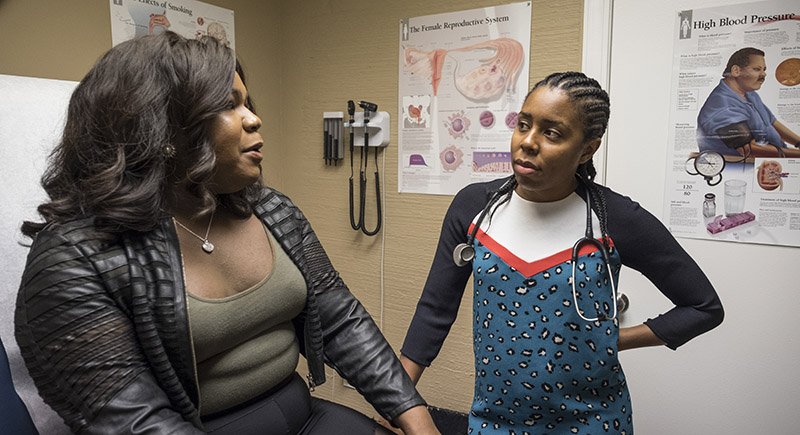
Photo by Nina Robinson/The Verbatim Agency/Getty Images.
“One of the techniques that we learned about early on from one of the residents is to say, ‘Many of my patients have experienced the effects of racism in health care. Do you have any experiences to share along those lines?’ Framing it as something that happened to other people might make others feel like they can speak up.”
— Juan Jaime De Zengotita, Medical Director at Southern Jamaica Plain Health Center in Boston, “In Focus: Reducing Racial Disparities in Health Care by Confronting Racism,” The Commonwealth Fund
Align organizational policies and activities
Even if our first four solutions were fully implemented, people’s health-related social needs would likely outstrip the public and philanthropic resources available to address them. Our final solution set highlights how health-sector institutions are pursuing policies that reduce the extent of unmet health-related social needs and deploy their clout to advocate for policies that would fill gaps and reduce inequities.
An estimated 16 million people worked in health care jobs in 2017. And in many communities, hospitals are the largest employers, giving them an important role in shaping people’s job quality and earnings. Health systems and hospitals can reduce the extent and severity of health-related social needs by raising workers’ wages and expanding their access to benefits.
Meanwhile, hospitals’ pricing, billing, and collection polices affect the financial well-being of patients and their families. Changing these practices, as some hospitals are doing, can minimize the adverse financial consequences of expensive hospital stays for low-income patients.
Hospitals can also support local economies and community development through their purchasing power.
- Henry Ford Health System, in partnership with Detroit Medical Center and Wayne State University, participates in Detroit’s “Live Local, Buy Local, Hire Local” initiative. In its first three years, this initiative helped more than 2,000 people move into Detroit’s Midtown neighborhoods, spent $16.5 million on locally owned businesses, and helped Henry Ford Health System hire 100 local residents.
Given their size, resources, and political influence, health-sector institutions and their leaders can join or even spearhead advocacy efforts to shape public policies and investments to address health-related social needs at the local, state, or federal levels.
- Greater Oregon Behavioral Health, Inc.—a partner in the eastern Oregon coordinated care organization—lobbied for changes in zoning codes in La Grande, Oregon, that allow development of so-called tiny cottages to increase affordable housing options.
- Health centers in Boston have been advocating for local investments and policy reforms to improve public transportation access and affordability so their patients can get to medical appointments.
- The American Academy of Pediatrics has advocated for the earned income tax credit, the child tax credit, higher minimum wages, and job-training programs to improve child and family health.
Finally, eliminating health inequities will require confronting and overturning racist policies and practices in education, employment, policing, health care delivery, and other areas.
- In one such effort, the Southern Jamaica Plain Health Center in Boston sought to understand and address health disparities between its white patients and patients of color by offering training to staff and community partners. The center developed a glossary to guide discussions about racial injustice, advocated for policy changes to address racial inequity, and produced a toolkit for addressing racial inequity in health care.
Health-Related Social Needs: Knowledge Priorities
Based on conversations with innovative thinkers and doers, we identified three areas where today’s health care payers, plans, and providers need new data and analysis to accelerate promising solutions for improving health equity by better addressing people’s health-related social needs.
“What’s lagging behind is clearer definitions around which social determinants of health have the biggest impact and which don’t. Where is the specific [return on investment] that the health care industry can lean on?”
Identify high-priority social needs
Health care providers and payers who want to strengthen how they tackle clients’ health-related social needs often lack information about the prevalence of those needs among the populations they serve. They also don’t have reliable evidence about the causal effects of unattended health-related social needs on health outcomes. By understanding which needs are most prevalent among their clients and which have the most impact on their health and health care costs, providers could target interventions to high-need groups and prioritize investments to reduce disparities in healthy life expectancy.
More specifically, health care changemakers could better prioritize specific social needs for experimental payment and delivery models. They could structure value-based payment arrangements and use managed care contracting to improve outcomes and reduce health inequities. And they could direct community benefit dollars toward investments that reduce health care costs and narrow disparities in healthy life expectancy. Achieving this would require
- refining and standardizing how plans and providers collect information on their clients’ health-related social needs to build population-specific databases on both the prevalence and patterns of needs,
- analyzing these databases to rigorously estimate the interactive impacts of social needs on outcomes and costs in health and other sectors, and
- collecting, synthesizing, and sharing research on the short- and long-term health effects of unmet social needs with the plans, providers, and policymakers who can apply them.
“Payers are interested in knowing about the actual evidence base for an intervention: Will it improve x, y, or z? If I have limited dollars, where should I invest them? What interventions should I invest in, from among the available options?”
Build an actionable evidence base of proven interventions
Health plans and payers that offer referrals and follow up to address their clients’ social needs or invest in community resource networks to meet those needs lack easy access to information on the costs and benefits of alternative approaches to screening, referral, and providing social services. They also need to know about any potential downsides to these activities (for providers, payers, or the people they serve) so they can avoid or mitigate unintended consequences. Assembling high-quality evidence about interventions for addressing health-related social needs would allow stakeholders to quickly identify cost-effective solutions for the people they serve and minimize duplicative and time-consuming research or experimentation. Building an actionable evidence base would require
- assembling and assessing evidence about the costs and effectiveness of different approaches for screening, referrals, and service delivery (this initial step will help identify the most urgent evidence gaps); and
- partnering with health care providers and payers to design demonstrations and conduct rigorous evaluations that build new evidence about how best to screen, provide referrals, and deliver services to different groups.
“We have a lot of good evidence about intervening within a sector, but where we could really see a payoff is across sectors. We have to get good numbers to convince officials at the state and federal levels to let the funds flow, which is a necessary condition to get these projects done.”
Assess strategies for integrating health, social services, and other systems
Communities, cities, and states are increasingly pursuing collaborative strategies that extend beyond the health care sector to address health-related social needs. But these efforts are difficult to justify and sustain without compelling evidence about the net positive returns they can expect to generate over time and across sectors. Moreover, each of these cross-sector efforts faces a host of design choices, from governance questions to legal and regulatory constraints, without guidance about the pros and cons of possible solutions. Three key knowledge-building investments would help policymakers and other stakeholders determine which approaches would work best in their settings and forecast the expected costs and returns to different sectors.
- Conduct comparative evaluations of existing approaches that synthesize and supplement the small amount of evaluation work available for individual cross-sector initiatives. Such an effort would answer questions about the formation, legal structures, and governance of collaboratives and analyze their effects on outcomes within and across sectors.
- Build rigorous process and outcome evaluations into new approaches, such as pay for success models.
- Provide evidence-based advice and technical assistance to collaborative efforts to better address health-related social needs, helping stakeholders find and apply the best available evidence on the organizational, regulatory, and financial questions they confront.
Based on the Health Catalyst Brief written by Genevieve M. Kenney, Timothy Waidmann, Laura Skopec, and Eva H. Allen.

